Lab-Grown Womb Models Reveal Secrets of Early Pregnancy and IVF Failures
A First Glimpse of Human Implantation—Outside the Body
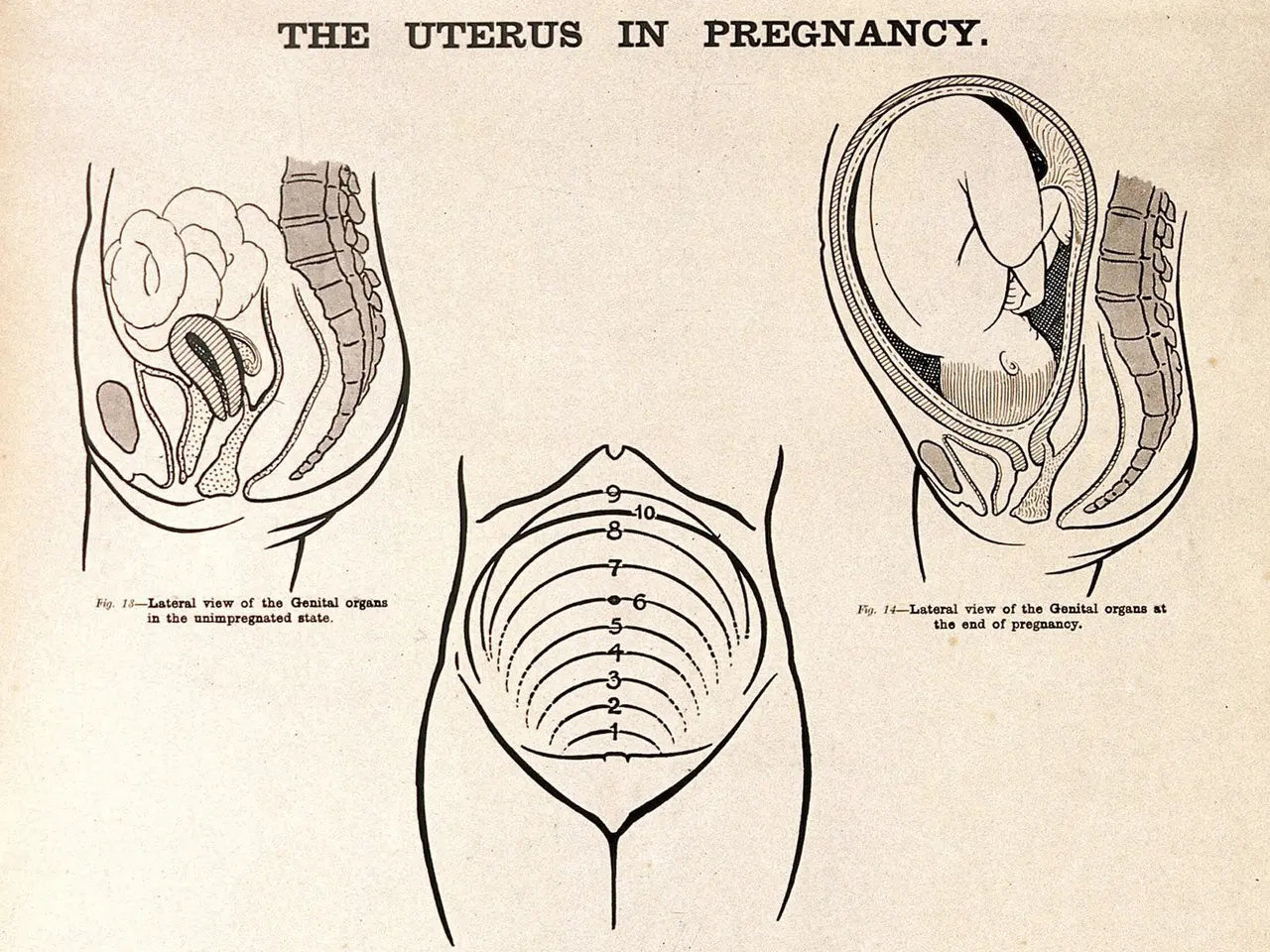
At first glance, it looks like the beginning of a human pregnancy: A spherical embryo gently presses into the receptive uterine lining, clings tightly, and burrows in as the first tendrils of what will become the placenta begin to form. This is implantation—the moment when pregnancy officially begins.
Except none of this is happening inside a body. These images were captured in a Beijing laboratory inside a microfluidic chip. In three research papers published in December by Cell Press, scientists describe what they call the most precise attempts yet to replicate the earliest moments of pregnancy in a lab. They obtained human embryos from in vitro fertilization (IVF) clinics and fused them with organoids—tiny, lab-grown structures made from endometrial cells that mimic the uterine lining.
Embryo Meets Organoid
Two studies from China and a third involving researchers from the UK, Spain, and the US demonstrate how scientists are using artificially engineered tissue to better understand early pregnancy—and potentially improve IVF success rates. "You have an embryo and an endometrial organoid together," says Jun Wu, a biologist at the University of Texas Southwestern Medical Center in Dallas, who contributed to both Chinese studies. "That's the overarching message of all three papers."
According to the publications, these 3D combinations are the most complete lab models yet of the first days of pregnancy and could help uncover why IVF so often fails. In every case, the experiments were halted once the embryos reached two weeks old—a legal and ethical limit that generally prohibits research on human embryos beyond 14 days.
Why Does IVF So Often Fail?
In a standard IVF procedure, an egg is fertilized in the lab and develops over several days into a spherical embryo called a blastocyst. This blastocyst is then transferred into a patient's uterus, with the hope that it will implant and eventually grow into a baby. But this is a common stumbling block—many patients learn their IVF cycle has failed because the embryo never implanted.
The new studies recreate this critical initial connection between mother and embryo in the lab. "IVF stands for in vitro fertilization, but now we're entering the era of in vitro implantation," says Matteo Molè, a biologist at Stanford University whose findings, co-authored with European colleagues, were published today. "Given that implantation is a major barrier, we have the potential to improve success rates if we can model it in the lab."
Normally, implantation is entirely invisible because it happens inside the uterus, says Hongmei Wang, a developmental biologist at the Beijing Institute for Stem Cell and Regenerative Medicine and a co-leader of the study. Wang often studies monkeys because she can interrupt their pregnancies to collect the necessary tissue. "We've always wanted to understand human embryo implantation, but we lacked the means to do it," she says. "The whole process happens inside the uterus."
Working with 50 Donated IVF Embryos
In the Beijing study, researchers examined around 50 donated IVF embryos but also conducted a thousand additional experiments using blastoids—lab-made models of early-stage human embryos derived from stem cells. Unlike real embryos, blastoids can be produced in large quantities and are subject to fewer ethical restrictions, making them a practical alternative for research.
"The question was: Now that we have these blastoids, what can we actually use them for?" says Leqian Yu, lead author of the report from the Beijing Institute. "The next logical step was implantation. But how do you even do that?" For the Peking-based team, the answer lay in constructing a soft silicone chamber with tiny channels to deliver nutrients and a space where a uterine organoid could grow. After that, blastoids—or real embryos—could be inserted through a window in the device, allowing the simulated pregnancy to begin. "The core question we want to answer is what that very first interaction between embryo and mother looks like," Yu explains. "I think this may be the first time we can observe the entire process."
Startups Racing to Harness Organoid Technology
Researchers have long sought to use organoids for this kind of work, and at least two startups have already secured funding to commercialize similar systems. In some cases, organoids are being marketed as a predictive tool for IVF success. Alongside Vienna-based Dawn Bio, there's Simbryo Technologies in Houston, which announced last November that it would offer "personalized" IVF outcome predictions for patients using blastoids and endometrial organoids.
For this test, doctors take a biopsy of the patient's uterine lining and grow it into an organoid. Blastoids are then added to assess whether the body would support a pregnancy. If the blastoids fail to implant, it could indicate that the patient's uterus is unreceptive—potentially explaining why IVF has not worked.
The Beijing team believes these pregnancy organoids could also help identify drugs to assist such patients. In their publication, they describe creating organoids from tissue taken from women who had experienced repeated IVF failures. They then tested 1,119 approved drugs on these samples to see if any improved outcomes.
Several showed promising effects. One chemical, avobenzone—a common sunscreen ingredient—boosted the likelihood of blastoid implantation from just 5% to around 25%. Yu says his center hopes to eventually launch a clinical trial once they find the right drug. For context, the maximum chance of a successful pregnancy per cycle in women under 30 is 25–35%, according to the Kinderwunsch Centrum Munich.
Making Simulated Pregnancies Even More Realistic
The Beijing group is working to refine their organoid system to make it even more lifelike. Currently, key cell types are missing, including immune cells and a blood supply. Yu says the next step for their chip-based device is to add blood vessels and miniature pumps, giving the organoids a rudimentary circulation system.
This could mean that blastoids or embryos might soon be cultured for longer periods, raising questions about how far researchers can push pregnancy in the lab. "I think this technology actually opens the door to extended culture," says Wu, noting that some view this research as a first step toward growing babies outside the body.
Still, Wu stresses that carrying a human to full term in a lab remains impossible for now. "This technology is certainly related to ectogenesis—the development outside the body," he says. "But I don't think it comes anywhere close to an artificial womb. That's still science fiction."